What is Oral Mucositis
Mucositis is painful inflammation and ulceration of the mucous membranes of the digestive tract, most commonly as an adverse effect of chemotherapy and radiotherapy treatments for cancer. Mucositis can occur anywhere along the gastrointestinal (GI) tract, but Oral mucositis refers to characteristic inflammation and ulcers occurring in the mouth. Oral mucositis is a common and mostly debilitating complication of cancer treatment.
About Oral Mucositis
Oral and gastrointestinal (GI) mucositis affects almost all patients undergoing high-dose chemotherapy and hematopoietic stem cell transplantation (HSCT), 80% of patients with head and neck malignancies are receiving radiotherapy, and 10% of patients receiving chemotherapy. There is a wide range of patients with. Alimentary tract mucositis increases mortality and morbidity and contributes to increased healthcare costs.
With most cancer treatments, approximately 5–15% of patients develop mucositis. However, with 5-fluorouracil (5-FU), up to 40% develop mucositis, and 10-15% develop grade 3-4 oral mucositis. [3] Irinotecan causes severe GI symptoms in more than 20% of patients. They are associated with mucositis. Seventy-five to eighty percent of bone marrow transplant recipients experience mucositis, of which oral mucositis is the most common and most debilitating, especially when melphalan is used. The patient can eat solid food in grade 3 oral mucositis and the patient can also consume liquids in grade 4.
In patients undergoing head and neck radiotherapy, pain and decreased oral function may persist long after cessation of therapy. Fractionated radiation doses increase the risk of mucositis in more than 70% of patients in most trials. HSCT recipients, meaning those who receive whole-body irradiation, have a particularly severe and long-lasting incidence of oral mucositis.
Symptoms of Oral Mucositis
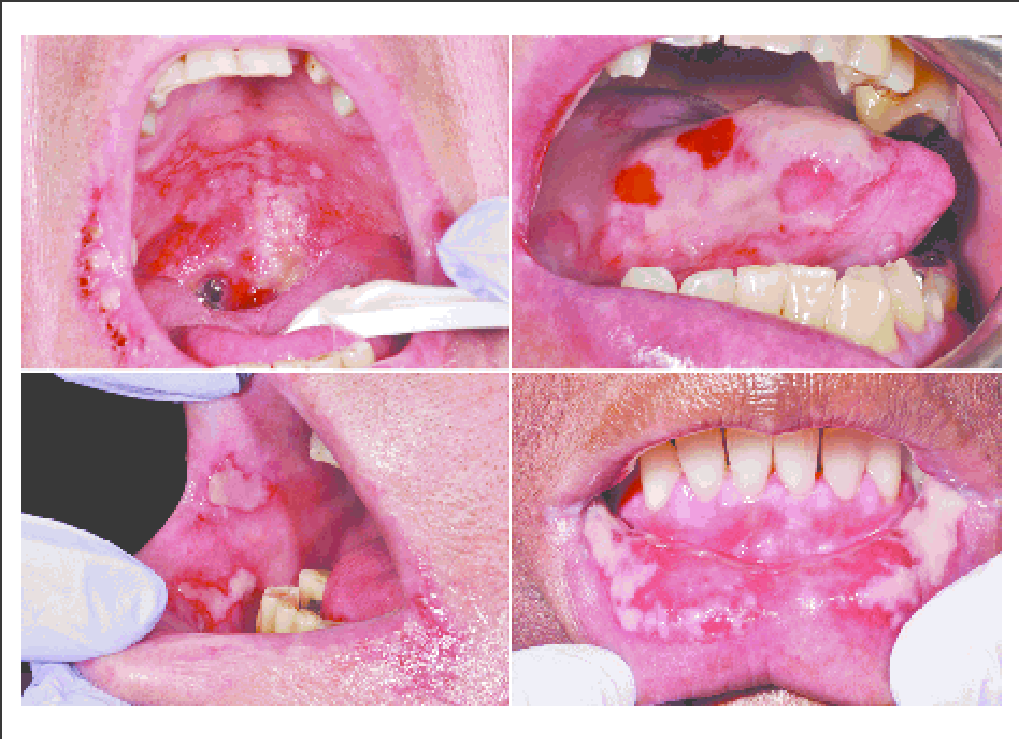
Oral mucositis can be severely painful. The intensity of pain is usually related to the extent of tissue damage. The pain is often described as a burning sensation with redness. Due to pain, the patient may have difficulty speaking, eating, or even opening the mouth. Changes in taste perception are common, especially for people receiving concomitant radiation therapy to the neck and mouth area. “Taste blindness”, or altered sense of taste, is a temporary condition caused by effects on the taste buds that are located mostly in the tongue. Sometimes, only partial recovery of taste occurs. Food tasting too sweet or bitter or having a persistent metallic taste are common complaints.
Another Factor
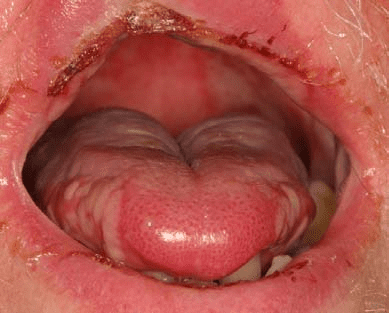
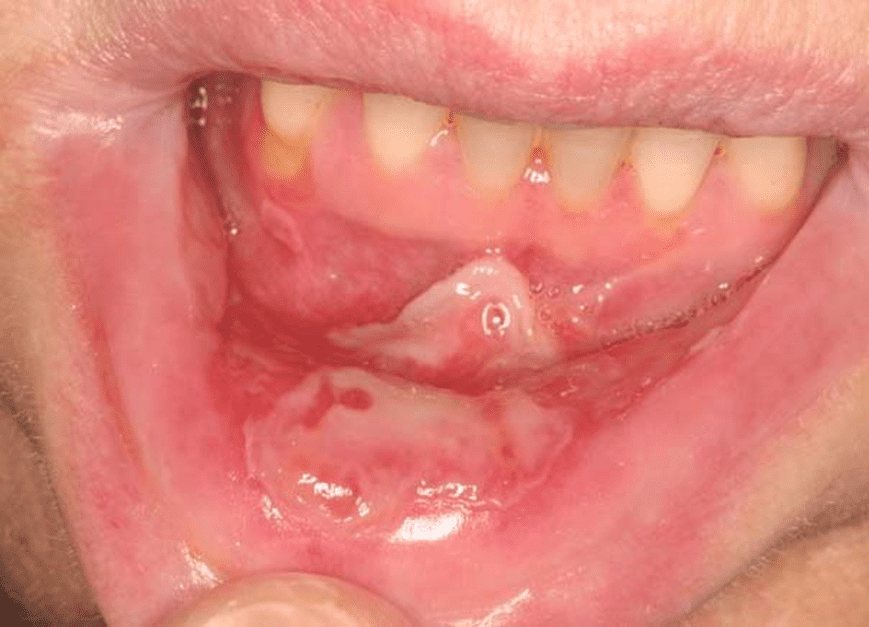
Cancer patients undergoing chemotherapy usually begin experiencing symptoms four to five days after starting treatment, peaking at about day 10 and then gradually improving over a few weeks. Mucositis associated with radiotherapy usually appears towards the end of the second week of treatment and can last for six to eight weeks. As a result of cell death in response to chemo- or radio-therapy, the mucosal lining of the mouth becomes thin, may become loose, and then become red, swollen, and ulcerated. The ulcer may be covered with a yellow-white fibrin clot called a pseudomembrane. Peripheral erythema is usually present. Ulcers can range from 0.5 cm to more than 4 cm.
Complications
Wounds or ulcers can become infected by viruses, bacteria, or fungi. Due to pain and loss of taste, it becomes difficult to eat food, which leads to weight loss. Ulcers can act as a site for local infection and a gateway for oral flora, which, in some cases, can lead to septicemia. Therefore, oral mucositis may be a dose-limiting condition, which may hinder a patient’s optimal cancer treatment plan and result in a lower chance of survival.
Causes of Oral Mucositis
- It usually involves a combination of chemotherapy, radiation, or surgery in cancer treatment. One of the unfortunate outcomes of these treatments is the development of painful mouth sores, which we call oral mucositis.
- High-dose chemotherapy, and high-dose radiation therapy localized to the head and neck region (for example for the treatment of head and neck cancer and lymphoma), are the main risk factors for the development of oral mucositis.
- These cancer treatments damage rapidly dividing cells, including the cells that make up the mucosa.
- High doses of radiation or chemotherapy or low doses of treatment in local areas in the entire body can affect your mouth or stomach organs.
These may also be other sporadic causes of oral mucositis which are very rare and insignificant. In a way, this can be said to be the first step in identifying the symptoms of the disease.
| Red, Shiny, swollen mouth and gums | Dry Mouth |
| Extra thick saliva | Mouth ulcers |
| Soft white spots of pus | Difficulty swallowing, talking, or eating |
| Bleeding | Layers of white mucus |
Five Stages of Oral mucositis
According to this image, it is much more understandable the five stages of oral mucositis:-
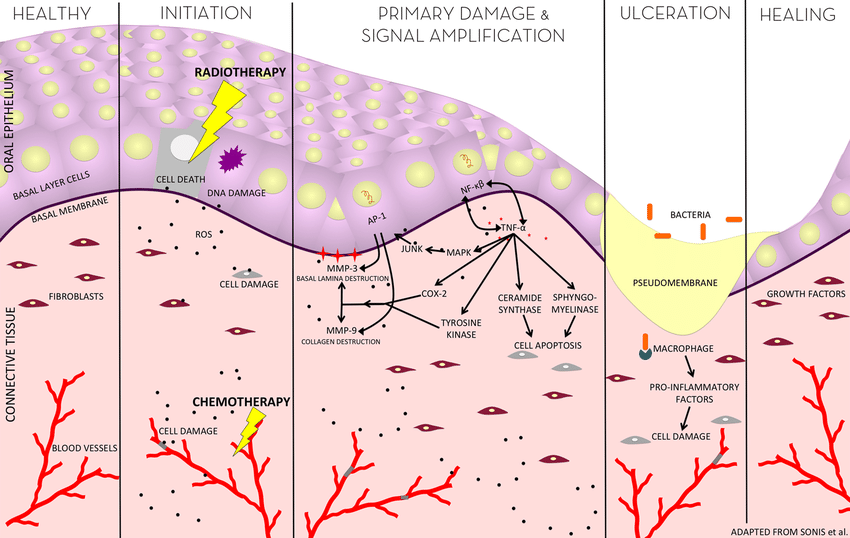
Prevention of Oral Mucositis
A 2015 Cochrane systematic review assessing the prevention of chemotherapy-induced oral mucositis concluded that oral cryotherapy leads to a large reduction in the incidence of oral mucositis of all severity in adults receiving 5-FU treatment for solid cancer. Evidence suggests a reduction in oral mucositis in adults receiving high-dose melphalan-based cancer treatment before hematopoietic stem cell transplantation, although there is uncertainty about the size of the reduction in this instance. No evidence was found for the use of this preventive measure in children. Oral cryotherapy involves placing rounded ice cubes in the mouth, which cools the oral tissues and causes vasoconstriction. This reduces blood flow to the area and, therefore, limits the amount of chemotherapy drugs delivered to the tissues.
Diagnosis of Mouth Mucositis
As we understand, mucositis is an expected side effect of cancer treatment. It is easy to diagnose based on your symptoms, medical history, and a look at the lump tissues. In the case of gastrointestinal mucositis, imaging tests may be needed to look at the tissues inside. Your healthcare provider may also want to test you for fungal infection of certain bacteria. Your healthcare provider can do this with a simple blood test.
Diagnosis is based on the symptoms the patient is experiencing and the appearance of mouth tissue after chemotherapy, bone marrow transplant, or radiotherapy. Red irritation-like lesions or ulcers throughout the mouth are sufficient to diagnose mucositis.
Treatment of Mucositis
Treatment of mucositis is mainly supportive. Oral hygiene is the foundation of treatment; Patients are encouraged to clean their mouth every four hours and at ill-timed, especially more frequently if the mucositis becomes disgusting. Mucositis will go away on its own after your cancer treatment course is finished. If you have chemotherapy, mucositis usually appears one to two weeks after treatment starts and resolves after one to six weeks. Mucositis appears two to three weeks after treatment begins and resolves within two to four weeks after your therapy ends if you have radiation therapy,
Water-soluble jelly can be used to lubricate the mouth. Salt mouthwash can soothe pain and keep food particles clean to prevent infection. Patients are also encouraged to drink plenty of fluids, at least three liters a day, and avoid alcohol. Citrus fruits, alcohol, and hot foods are known to aggravate mucositis lesions. Medicated mouthwashes such as chlorhexidine gluconate and gummy lidocaine can be used to relieve pain. However, caution must be exercised as high doses of viscous lidocaine have adverse effects. One study reported that lidocaine has potential toxicity; When it was tested on patients with oral mucositis undergoing bone marrow transplantation, lidocaine anesthetic mouthwash was found to be absorbed systemically.